The surgical technique of
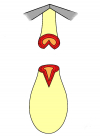
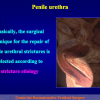
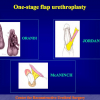
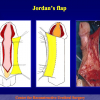
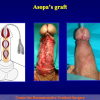
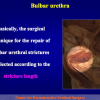
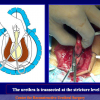
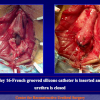
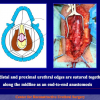
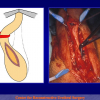
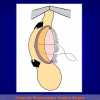
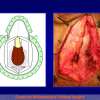
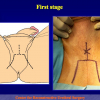
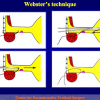
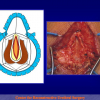
“End-to-end anastomosis” is made by transecting the urethra at the level of the stricture site, removing the scar tissue and performing a direct anastomosis between the two urethral edges. This surgical technique is one of the fist operations described in the repair of urethral strictures
|
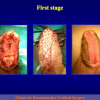
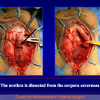
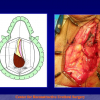
Figure 1
|
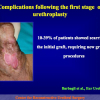
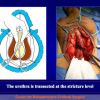
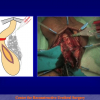
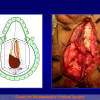
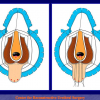
Figure 2
|
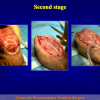
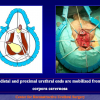
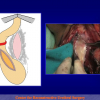
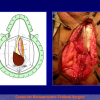
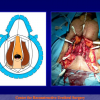
Figure 3
|
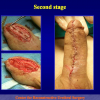
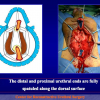
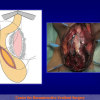
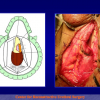
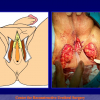
Figure 4
|
Basically, there are two basic types of End-to-end anastomosis:
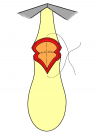
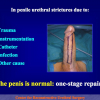
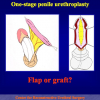
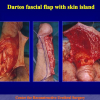
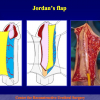
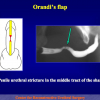
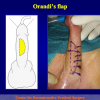
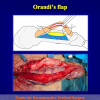
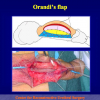
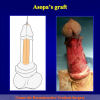
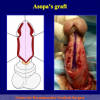
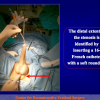
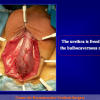
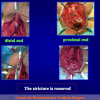
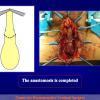
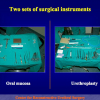
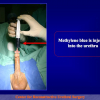
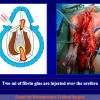
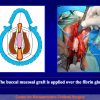
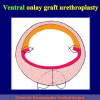
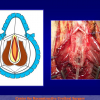
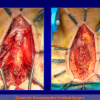
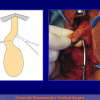
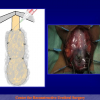
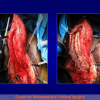
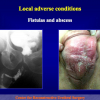
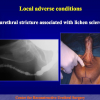
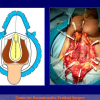
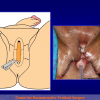
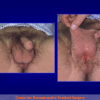
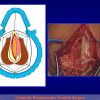
- End-to-end anastomosis. Using this technique, the scar tissue involving the stricture is completely removed and the new urethral lumen is made on healthy tissue with an adequate caliber (figures 1,2).
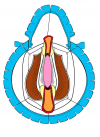
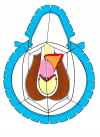
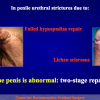
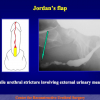
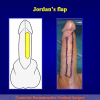
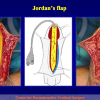
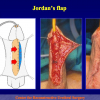
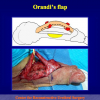
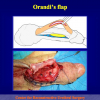
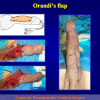
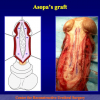
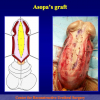
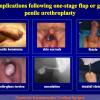
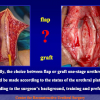
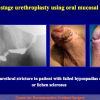
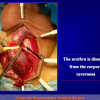
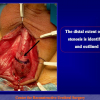
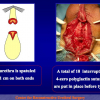
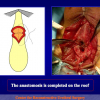
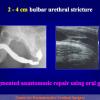
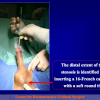
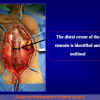
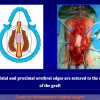
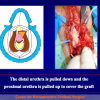
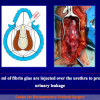
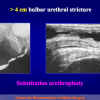
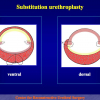
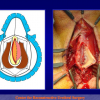
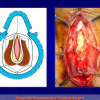
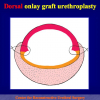
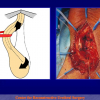
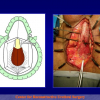
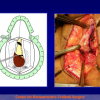
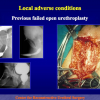
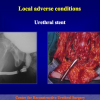
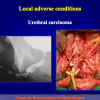
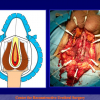
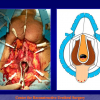
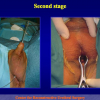
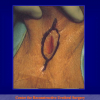
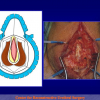
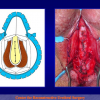
- End-to-end anastomosis with skin or oral mucosal graft. Using this technique, the scar tissue involving the stricture is completely removed and the new urethral lumen is made on healthy tissue with an adequate caliber over the graft (figures 3,4).
The surgical technique of End-to-end anastomosis is generally suggested in the following cases:
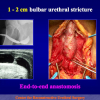
- patients with traumatic bulbar urethral strictures, not more than 2 cm in length.
- patients who had undergone previous failed surgical attempt to repair urethral strictures showing a recurrent fibrous stricture not more than 2 cm in length.
Lecture n° 1:
Penile and bulbar urethroplasty Surgical techniques and results
Hong Kong Urological Association Urethroplasty Workshop Division of Urology – Tuen Mun Hospital
February 9 – 10, 2009
Hong Kong |
|

scarica PDF |
Article n° 1
Barbagli G, Palminteri E, Bartoletti R, Selli C, Rizzo M.
Long-term results of anterior and posterior urethroplasty with actuarial evaluation of the success rates.
J Urol. 1997 Oct;158(4):1380-2.
Purpose: We analyzed the long-term results of different urethroplasty techniques.
Materials and Methods: We performed a retrospective review of 98 patients who underwent different procedures for anterior (78) and posterior (20) urethral strictures. Mean followup was 53 months. A total of 20 patients underwent end-to-end anastomosis (group 1), 30 underwent 1-stage procedures (group 2), 28 underwent 2-stage procedures (group 3), and 20 underwent bulboprostatic anastomosis (group 4). The results were analyzed using Kaplan-Meier curves and log rank test.
Results: The success rate was 95% for group 1, 93.4% for group 2, 78.6% for group 3, and 70% for group 4. Statistical evaluation of the actuarial success rates failed to show significant differences among the 4 groups.
Conclusions: The stricture recurrences were uniformly distributed over time. Urethroplasty patients must be followed for the rest of their lives.
Article n° 2
Barbagli G, Palminteri E, Lazzeri M, Guazzoni G, Turini D.
Long-term outcome of urethroplasty after failed urethrotomy versus primary repair.
J Urol. 2001 Jun;165(6 Pt 1):1918-9.
Purpose: A urethral stricture recurring after repeat urethrotomy challenges even a skilled urologist. To address the question of whether to repeat urethrotomy or perform open reconstructive surgery, we retrospectively review a series of 93 patients comparing those who underwent primary repair versus those who had undergone urethrotomy and underwent secondary treatment.
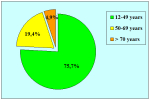
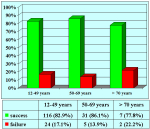
Materials and Methods: From 1975 to 1998, 93 males between age 13 and 78 years (mean 39) underwent surgical treatment for bulbar urethral stricture. In 46 (49%) of the patients urethroplasty was performed as primary repair, and in 47 (51%) after previously failed urethrotomy. The strictures were localized in the bulbous urethra without involvement of penile or membranous tracts. The etiology was ischemic in 37 patients, traumatic in 23, unknown in 17 and inflammatory in 16. To simplify evaluation of the results, the clinical outcome was considered either a success or a failure at the time any postoperative procedure was needed, including dilation.
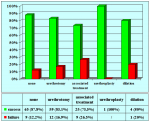
Results: In our 93 patients primary urethroplasty had a final success rate of 85%, and after failed urethrotomy 87%. Previously failed urethrotomy did not influence the long-term outcome of urethroplasty. The long-term results of different urethroplasty techniques had a final success rate ranging from 77% to 96%.
Conclusions: We conclude that failed urethrotomy does not condition the long-term result of surgical repair. With extended followup, the success rate of urethroplasty decreases with time but it is in fact still higher than that of urethrotomy.
Article n° 3
Guido Barbagli, Michele De Angelis, Giuseppe Romano and Massimo Lazzeri
Long-Term Followup of Bulbar End-to-End Anastomosis: A Retrospective Analysis of 153 Patients in a Single Center Experience
J Urol 2007; 178: 2470-2473
Purpose: We performed a retrospective evaluation and statistical analysis of outcome in patients who underwent bulbar end-to-end anastomosis.
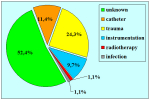
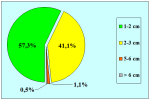
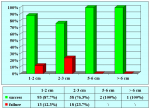
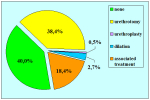
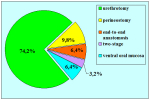
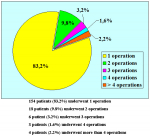
Materials and Methods: We reviewed 153 patients with an average age of 39 years who underwent bulbar end-to-end anastomosis between 1988 and 2006. Mean followup was 68 months. Stricture etiology was unknown (62.7%), catheter (14.4%), blunt perineal trauma (11.7%), instrumentation (9.8%), radiotherapy (0.7%) and infection (0.7%). Stricture length was 1 to 2 cm (in 59.5%), 2 to 3 cm (37.9%), 3 to 4 cm (1.9%) or 4 to 5 cm (0.7%). A total of 90 patients (59%) underwent dilation, internal urethrotomy, urethroplasty or multiple procedures before being referred to our center. Clinical outcome was considered a treatment failure when any postoperative instrumentation was needed. The prevalence of postoperative sexual dysfunction was investigated using a nonvalidated questionnaire.
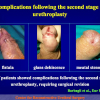
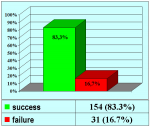
Results: Of 153 cases 139 (90.8%) were successful and 14 (9.2%) were treatment failures. Treatment failure was managed with urethrotomy in 9 cases, end-to-end anastomosis in 2, buccal mucosal graft urethroplasty in 1 and 2-stage repair in 2. Of 14 cases of failure 12 had a satisfactory final outcome, 1 is still waiting for the second stage of urethroplasty and 1 underwent definitive perineostomy. There were 14 patients (23.3%) who experienced ejaculatory dysfunction, 1 (1.6%) a cold glans during erection, 7 (11.6%) a glans that was neither full nor swollen during erection and 11 (18.3%) had decreased glans sensitivity. No patients complained of penile chordee or impotence.
Conclusions: Bulbar end-to-end anastomosis has a success rate of 90.8%. Most patients were satisfied with the surgical outcome despite postoperative complications such as ejaculatory dysfunction, a glans that was neither full nor swollen during erection, or decreased penile sensitivity.
1. Question: What kind of anesthesia is used for this surgery?
Answer: General anesthesia with oro-tracheal intubation.
2. Question: How many hours does the surgery take?
Answer: About 2 hours.
3. Question: Are there any risks concerning erection, fertility and urinary incontinence after the surgery?
Answer: No, there aren’t.
4. Question: How many days of hospital recovery are expected following the surgery?
Answer: In general, from 5 to 7 days.
5. Question: How long will I have to use a catheter after the surgery?
Answer: The urethral catheter must stay in place for four weeks after the surgery, when the first post-operative voiding urethrography is done.
6. Question: Are there any particular recommendations during convalescence?
Answer: During convalescence, the use antibiotics until the catheter is removed is suggested. Avoiding long car trips, as well as heavy labor and sexual and sports activities are also suggested.
7. Question: When will I be able to resume my working, sexual and sports activities?
Answer: All these activities can be gradually resumed about 30 days after the removal of the catheter.
8. Question: Can I ride a bike or a motorcycle immediately after the surgery?
Answer: It is not recommended to ride bikes, motorcycles or horses after the surgery.
9. Question: What kinds of foods and drinks should be avoided after the surgery?
Answer: Beer and sparkling wines should be avoided, as well as large quantities of chocolate, cocoa, nuts and shellfish.
Surgical Technique: step by step