The surgical technique of “End-to-end anastomosis” is made by transecting the urethra at the level of the stricture site, removing the scar tissue and performing a direct anastomosis between the two urethral edges. This surgical technique is one of the fist operations described in the repair of urethral strictures
|
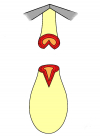
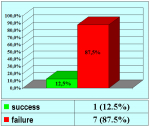
Figure 1 |
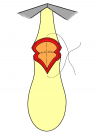
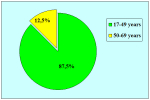
Figure 2 |
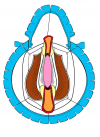
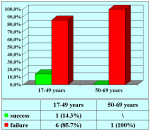
Figure 3 |
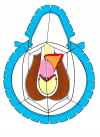
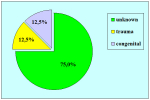
Figure 4 |
Basically, there are two basic types of End-to-end anastomosis:
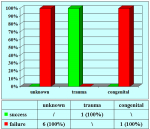
- End-to-end anastomosis. Using this technique, the scar tissue involving the stricture is completely removed and the new urethral lumen is made on healthy tissue with an adequate caliber (figures 1,2).
- End-to-end anastomosis with skin or oral mucosal graft. Using this technique, the scar tissue involving the stricture is completely removed and the new urethral lumen is made on healthy tissue with an adequate caliber over the graft (figures 3,4).
The surgical technique of End-to-end anastomosis is generally suggested in the following cases:
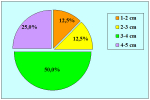
- patients with traumatic bulbar urethral strictures, not more than 2 cm in length.
- patients who had undergone previous failed surgical attempt to repair urethral strictures showing a recurrent fibrous stricture not more than 2 cm in length.
Article n° 1
Barbagli G, Selli C, di Cello V, Mottola A.
A one-stage dorsal free-graft urethroplasty for bulbar urethral strictures.
Br J Urol. 1996 Dec;78(6):929-32
Article n° 2
Barbagli G, Selli C, Tosto A, Palminteri E.
Dorsal free graft urethroplasty
J Urol. 1996 Jan;155(1):123-6
Article n° 3
Barbagli G, Palminteri E, Rizzo M.
Dorsal onlay graft urethroplasty using penile skin or buccal mucosa in adult bulbourethral strictures.
J Urol. 1998 Oct;160(4):1307-9
Article n° 4
Barbagli G, Palminteri E, Lazzeri M, Guazzoni G, Turini D.
Long-term outcome of urethroplasty after failed urethrotomy versus primary repair
J Urol. 2001 Jun;165(6 Pt 1):1918-9
Article n° 5
Barbagli G, Palminteri E, Guazzoni G, Montorsi F, Turini D, Lazzeri M.
Interim outcomes of dorsal skin graft bulbar urethroplasty.
JUrol. Volume 172, Issue 4, Pages 1365-1367 (October 2004)
Article n° 6
Guido Barbagli, Giuseppe Morgia, Massimo Lazzeri
Dorsal Onlay Skin Graft Bulbar Urethroplasty: Long-Term Follow-Up
Eur. Urol. 2008,53:628 – 634
Barbagli G, Selli C, di Cello V, Mottola A.
A one-stage dorsal free-graft urethroplasty for bulbar urethral strictures.
Br J Urol. 1996 Dec;78(6):929-32
Article n° 2
Barbagli G, Selli C, Tosto A, Palminteri E.
Dorsal free graft urethroplasty
J Urol. 1996 Jan;155(1):123-6
Article n° 3
Barbagli G, Palminteri E, Rizzo M.
Dorsal onlay graft urethroplasty using penile skin or buccal mucosa in adult bulbourethral strictures.
J Urol. 1998 Oct;160(4):1307-9
Article n° 4
Barbagli G, Palminteri E, Lazzeri M, Guazzoni G, Turini D.
Long-term outcome of urethroplasty after failed urethrotomy versus primary repair
J Urol. 2001 Jun;165(6 Pt 1):1918-9
Article n° 5
Barbagli G, Palminteri E, Guazzoni G, Montorsi F, Turini D, Lazzeri M.
Interim outcomes of dorsal skin graft bulbar urethroplasty.
JUrol. Volume 172, Issue 4, Pages 1365-1367 (October 2004)
Article n° 6
Guido Barbagli, Giuseppe Morgia, Massimo Lazzeri
Dorsal Onlay Skin Graft Bulbar Urethroplasty: Long-Term Follow-Up
Eur. Urol. 2008,53:628 – 634
1. Question: What kind of anesthesia is used for this surgery?
Answer: General anesthesia with oro-tracheal intubation.
2. Question: How many hours does the surgery take?
Answer: About 2 hours.
3. Question: Are there any risks concerning erection, fertility and urinary incontinence after the surgery?
Answer: No, there aren’t.
4. Question: How many days of hospital recovery are expected following the surgery?
Answer: In general, from 5 to 7 days.
5. Question: How long will I have to use a catheter after the surgery?
Answer: The urethral catheter must stay in place for four weeks after the surgery, when the first post-operative voiding urethrography is done.
6. Question: Are there any particular recommendations during convalescence?
Answer: During convalescence, the use antibiotics until the catheter is removed is suggested. Avoiding long car trips, as well as heavy labor and sexual and sports activities are also suggested.
7. Question: When will I be able to resume my working, sexual and sports activities?
Answer: All these activities can be gradually resumed about 30 days after the removal of the catheter.
8. Question: Can I ride a bike or a motorcycle immediately after the surgery?
Answer: It is not recommended to ride bikes, motorcycles or horses after the surgery.
9. Question: What kinds of foods and drinks should be avoided after the surgery?
Answer: Beer and sparkling wines should be avoided, as well as large quantities of chocolate, cocoa, nuts and shellfish.
Answer: General anesthesia with oro-tracheal intubation.
2. Question: How many hours does the surgery take?
Answer: About 2 hours.
3. Question: Are there any risks concerning erection, fertility and urinary incontinence after the surgery?
Answer: No, there aren’t.
4. Question: How many days of hospital recovery are expected following the surgery?
Answer: In general, from 5 to 7 days.
5. Question: How long will I have to use a catheter after the surgery?
Answer: The urethral catheter must stay in place for four weeks after the surgery, when the first post-operative voiding urethrography is done.
6. Question: Are there any particular recommendations during convalescence?
Answer: During convalescence, the use antibiotics until the catheter is removed is suggested. Avoiding long car trips, as well as heavy labor and sexual and sports activities are also suggested.
7. Question: When will I be able to resume my working, sexual and sports activities?
Answer: All these activities can be gradually resumed about 30 days after the removal of the catheter.
8. Question: Can I ride a bike or a motorcycle immediately after the surgery?
Answer: It is not recommended to ride bikes, motorcycles or horses after the surgery.
9. Question: What kinds of foods and drinks should be avoided after the surgery?
Answer: Beer and sparkling wines should be avoided, as well as large quantities of chocolate, cocoa, nuts and shellfish.
| Up-to-date to 12-31-2021 | |||

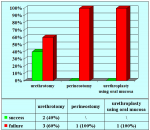
Summarizing table |
|||