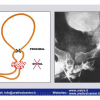
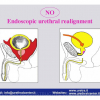
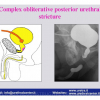
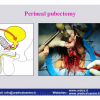
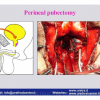
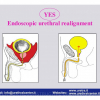
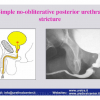
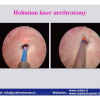
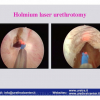
| The male urethra is divided into the anterior and posterior urethra. The posterior urethra consists of the segment that extends from the bladder neck to the distal external urethral sphincter and can be divided into the prostatic urethra and the membranous urethra. The anterior urethra extends from the distal external urethral sphincter to the external urinary meatus and is divided into the bulbar, penile and navicularis urethra. The posterior urethra includes the two urinary sphincters, at the level of the bladder neck (proximal urinary sphincter) and at the level of membranous urethra (distal urinary sphincter). |
Lecture n° 1:
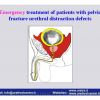
| Initial evaluation and management of the patient with pelvic fracture urethral distraction defects (PFUDD) 1 December 2007 Rome — Italy |
 Download PDF |
|
|
|
||
| Lecture n° 2: | ||
| Incontinence following pelvic trauma 23rd Annual EAU Congress Sub-plenary Session on Male urinary incontinence March 26-29, 2008 Milan — Italy |
 Download PDF |
|
|
|
||
| Lecture n° 3: | ||
| Posterior Urethroplasty III Simposio Internacional de Cirurgia Urologica Reconstrutora April 11-12, 2008 Rio de Janeiro-Brazil |
 Download PDF |
|
|
|
||
| Lecture n° 4: | ||
| Chirurgia dell’uretra posteriore Mantova — Italy |
 Download PDF |
|
|
|
||
| Lecture n° 5: | ||
| Traumatic posterior urethral disruption. Pelvic fracture urethral distraction defects Congress of French Association of Urology ESU COURSE: Trauma in Urology November, 20 — 2008 Paris – France |
 Download PDF |
|
|
|
||
| Lecture n° 6: | ||
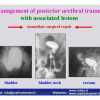
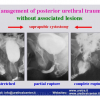
| Acute management of posterior urethral trauma. What are the options and what is the current consensus Muljibhai Patel Urological Hospital “URETHROPLASTY” July 19 – 20, 2012 Nadiad – Gujarat – India |
 Download PDF |
|
|
|
||
| Lecture n° 7: | ||
| Emergency and delayed treatment of patients with pelvic fracture urethral distraction defects 9th Conference of the Arab Association of Urology 7th International Conference of Jordanian Association of Urological Surgeons November 22 — 24, 2011 Amman – Jordan |
 Download PDF |
Article n° 1
Urethral trauma: radiological aspects and treatment options.
J Trauma. 1987 Mar; 27(3):256-61
Article n° 2
Posterior urethroplasty in children.
Eur Urol. 1987;13(1-2):110-5.
Article n° 3
Long-term results of anterior and posterior urethroplasty with actuarial evaluation of the success rates.
J Urol. 1997 Oct;158(4):1380-2.
Articolo n° 4
History and Evolution of Transpubic Urethroplasty:
A Lesson for Young Urologists in Training
Eur Urol 2007; 52:1290 — 1292
Urethral trauma: radiological aspects and treatment options.
J Trauma. 1987 Mar; 27(3):256-61
Article n° 2
Posterior urethroplasty in children.
Eur Urol. 1987;13(1-2):110-5.
Article n° 3
Long-term results of anterior and posterior urethroplasty with actuarial evaluation of the success rates.
J Urol. 1997 Oct;158(4):1380-2.
Articolo n° 4
History and Evolution of Transpubic Urethroplasty:
A Lesson for Young Urologists in Training
Eur Urol 2007; 52:1290 — 1292
1. Question: What kind of anesthesia is used for this surgery?
Answer: General anesthesia with oro-tracheal intubation.
2. Question: How many hours does the surgery take?
Answer: About 3 hours.
3. Question: Are there any risks concerning erection, fertility and continence after the surgery?
Answer: If the bladder neck was not injured during the pelvic trauma or emergency treatment, the posterior urethroplasty is safe with regard to urinary continence. The preoperative radiological study provides sure information about the integrity of the bladder neck. Patients with pelvic trauma and urethral rupture may show some degree of erectile dysfunction, due to urethral disruption. Posterior urethroplasty may cause erectile dysfunction. If the bladder neck is not damaged the fertility is not at risk.
4. Question: How many days of hospital recovery are expected following the surgery?
Answer: In general, from 5 to 7 days.
5. Question: How long will I have to use a urethral catheter and suprapubic tube after the surgery?
Answer: The urethral catheter must stay in place for four weeks following surgery, when the first post-operative voiding urethrography is done. The suprapubic tube must stay in place for two months following surgery, when the second post-operative voiding urethrography is done.
6. Question: Are there any particular recommendations during convalescence?
Answer: During convalescence, antibiotic use is suggested until the catheter is removed. It is also suggested that long car trips be avoided, as well as heavy labor, sexual activity and sports.
7. Question: When will I be able to resume work, sexual activity and sports?
Answer: All these activities can be gradually resumed after the removal of the catheter.
8. Question: Can I ride a bike or a motorcycle immediately after the surgery?
Answer: It is not recommended to ride bikes, motorcycles or horses after the surgery.
9. Question: What kinds of foods and drinks should be avoided after the surgery?
Answer: Beer and sparkling wines should be avoided, as well as large quantities of chocolate, cocoa, nuts and shellfish.
Answer: General anesthesia with oro-tracheal intubation.
2. Question: How many hours does the surgery take?
Answer: About 3 hours.
3. Question: Are there any risks concerning erection, fertility and continence after the surgery?
Answer: If the bladder neck was not injured during the pelvic trauma or emergency treatment, the posterior urethroplasty is safe with regard to urinary continence. The preoperative radiological study provides sure information about the integrity of the bladder neck. Patients with pelvic trauma and urethral rupture may show some degree of erectile dysfunction, due to urethral disruption. Posterior urethroplasty may cause erectile dysfunction. If the bladder neck is not damaged the fertility is not at risk.
4. Question: How many days of hospital recovery are expected following the surgery?
Answer: In general, from 5 to 7 days.
5. Question: How long will I have to use a urethral catheter and suprapubic tube after the surgery?
Answer: The urethral catheter must stay in place for four weeks following surgery, when the first post-operative voiding urethrography is done. The suprapubic tube must stay in place for two months following surgery, when the second post-operative voiding urethrography is done.
6. Question: Are there any particular recommendations during convalescence?
Answer: During convalescence, antibiotic use is suggested until the catheter is removed. It is also suggested that long car trips be avoided, as well as heavy labor, sexual activity and sports.
7. Question: When will I be able to resume work, sexual activity and sports?
Answer: All these activities can be gradually resumed after the removal of the catheter.
8. Question: Can I ride a bike or a motorcycle immediately after the surgery?
Answer: It is not recommended to ride bikes, motorcycles or horses after the surgery.
9. Question: What kinds of foods and drinks should be avoided after the surgery?
Answer: Beer and sparkling wines should be avoided, as well as large quantities of chocolate, cocoa, nuts and shellfish.
| Up-to-date to 12-31-2021 | |||

PDF Summarizing table |
|||