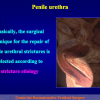
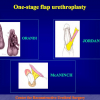
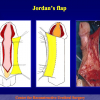
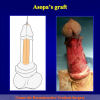
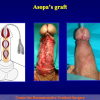
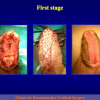
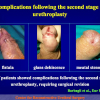
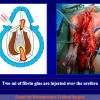
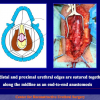
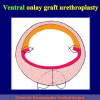
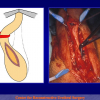
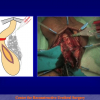
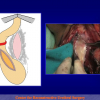
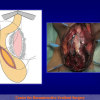
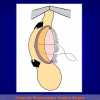
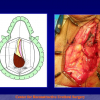
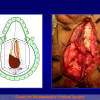
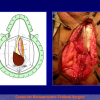
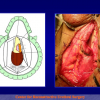
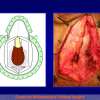
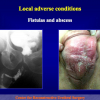
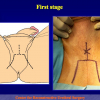
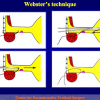
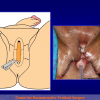
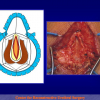
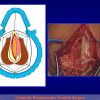
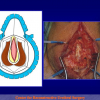
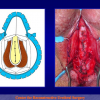
The surgical technique of “Two-stage Urethroplasty” is conducted in two operations performed at different times.
|
Figure 1 |
Figure 2 |
Figure 3 |
Figure 4 |
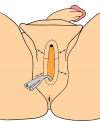
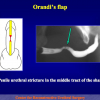
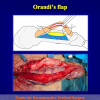
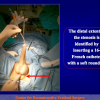
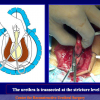
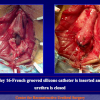
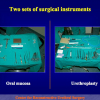
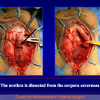
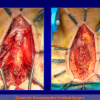
During the first operation, the urethra is opened and a perineal urethrostomy (figure 1).
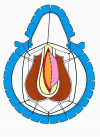
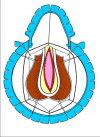
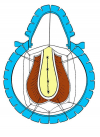
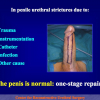
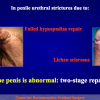
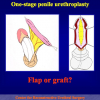
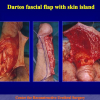
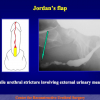
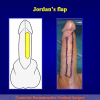
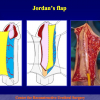
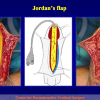
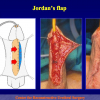
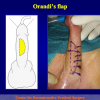
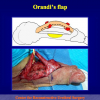
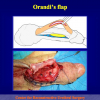
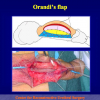
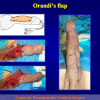
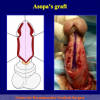
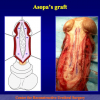
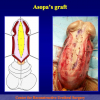
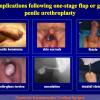
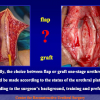
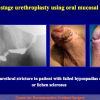
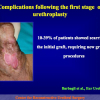
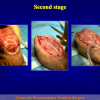
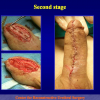
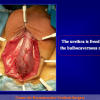
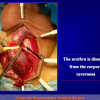
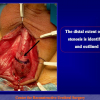
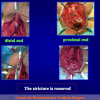
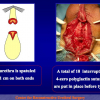
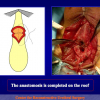
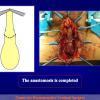
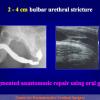
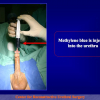
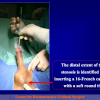
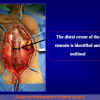
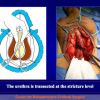
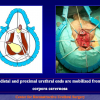
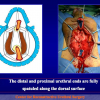
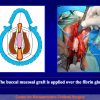
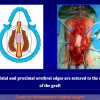
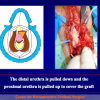
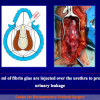
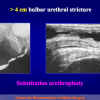
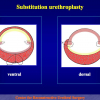
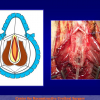
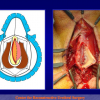
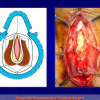
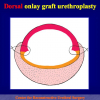
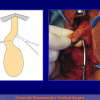
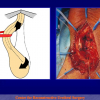
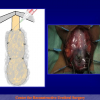
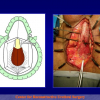
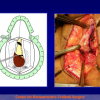
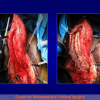
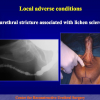
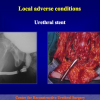
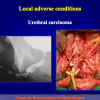
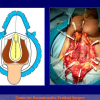
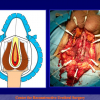
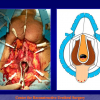
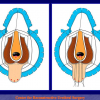
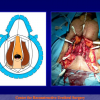
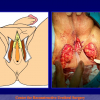
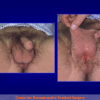
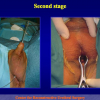
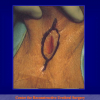
One year later, the perineal urethrostomy is closed (figure 2-3-4) and the patient is again able to void through the external urinary meatus.
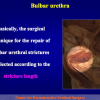
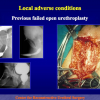
The surgical technique of Two-stage urethroplasty is generally suggested in the patients with complex urethral strictures.
Lecture n° 1:
| Uretroplastia en dos tiempos ¿cómo y cuándo ? 51 Curso de Urologia Fundació Puigevert 18 – 20 de octubre 2006 Barcelona — Spain |
 Download PDF |
|
|
|
||
| Lecture n° 2: | ||
| Penile and bulbar urethroplasty Surgical techniques and results Hong Kong Urological Association Urethroplasty Workshop Division of Urology – Tuen Mun Hospital Hong Kong February 9 — 10, 2009 |
 Download PDF |
Article n° 1
Barbagli G, Palminteri E, Bartoletti R, Selli C, Rizzo M.
Long-term results of anterior and posterior urethroplasty with actuarial evaluation of the success rates.
J Urol. 1997 Oct;158(4):1380-2.
Article n° 2
Barbagli G, Palminteri E, Lazzeri M, Guazzoni G, Turini D.
Long-term outcome of urethroplasty after failed urethrotomy versus primary repair.
J Urol. 2001 Jun;165(6 Pt 1):1918-9
Article n° 3
Palminteri E, Lazzeri M, Guazzoni G, Turini D, Barbagli G.
New 2-stage buccal mucosal graft urethroplasty.
J Urol. 2002 Jan;167(1):130-2
Article n° 4
Barbagli G., Guazzoni G., Lazzeri M.
One-Stage bulbar urethroplasty: Retrospective analisys of the results in 375 patients
Eur Urol 2008; 53:828 — 33
Barbagli G, Palminteri E, Bartoletti R, Selli C, Rizzo M.
Long-term results of anterior and posterior urethroplasty with actuarial evaluation of the success rates.
J Urol. 1997 Oct;158(4):1380-2.
Article n° 2
Barbagli G, Palminteri E, Lazzeri M, Guazzoni G, Turini D.
Long-term outcome of urethroplasty after failed urethrotomy versus primary repair.
J Urol. 2001 Jun;165(6 Pt 1):1918-9
Article n° 3
Palminteri E, Lazzeri M, Guazzoni G, Turini D, Barbagli G.
New 2-stage buccal mucosal graft urethroplasty.
J Urol. 2002 Jan;167(1):130-2
Article n° 4
Barbagli G., Guazzoni G., Lazzeri M.
One-Stage bulbar urethroplasty: Retrospective analisys of the results in 375 patients
Eur Urol 2008; 53:828 — 33
1. Question: What kind of anesthesia is used for this surgery?
Answer: General anesthesia with nasal or oro-tracheal intubation.
2. Question: How many hours does the surgery take?
Answer: About 2 hours for the first operation and one hour for the second operation.
3. Question: Are there any risks concerning erection, fertility and urinary incontinence after the surgery?
Answer: No, there aren’t.
4. Question: How many days of hospital recovery are expected following the surgery?
Answer: In general, from 5 to 7 days for both operations.
5. Question: How long will I have to use a catheter after the surgery?
Answer: The urethral catheter must stay in place for two weeks following the first operation, and for four weeks following the second operation, when the first post-operative voiding urethrography is done.
6. Question: Are there any particular recommendations during convalescence?
Answer: During convalescence, the use antibiotics until the catheter is removed is suggested. Avoiding long car trips, as well as heavy labor and sexual and sports activities are also suggested.
7. Question: When will I be able to resume my working, sexual and sports activities?
Answer: All these activities can be gradually resumed about 30 days after the removal of the catheter.
8. Question: Can I ride a bike or a motorcycle immediately after the surgery?
Answer: It is not recommended to ride bikes, motorcycles or horses after the surgery.
9. Question: What kinds of foods and drinks should be avoided after the surgery?
Answer: Beer and sparkling wines should be avoided, as well as large quantities of chocolate, cocoa, nuts and shellfish.
Answer: General anesthesia with nasal or oro-tracheal intubation.
2. Question: How many hours does the surgery take?
Answer: About 2 hours for the first operation and one hour for the second operation.
3. Question: Are there any risks concerning erection, fertility and urinary incontinence after the surgery?
Answer: No, there aren’t.
4. Question: How many days of hospital recovery are expected following the surgery?
Answer: In general, from 5 to 7 days for both operations.
5. Question: How long will I have to use a catheter after the surgery?
Answer: The urethral catheter must stay in place for two weeks following the first operation, and for four weeks following the second operation, when the first post-operative voiding urethrography is done.
6. Question: Are there any particular recommendations during convalescence?
Answer: During convalescence, the use antibiotics until the catheter is removed is suggested. Avoiding long car trips, as well as heavy labor and sexual and sports activities are also suggested.
7. Question: When will I be able to resume my working, sexual and sports activities?
Answer: All these activities can be gradually resumed about 30 days after the removal of the catheter.
8. Question: Can I ride a bike or a motorcycle immediately after the surgery?
Answer: It is not recommended to ride bikes, motorcycles or horses after the surgery.
9. Question: What kinds of foods and drinks should be avoided after the surgery?
Answer: Beer and sparkling wines should be avoided, as well as large quantities of chocolate, cocoa, nuts and shellfish.
| Up-to-date to 12-31-2021 | |||

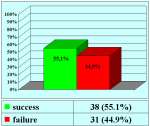
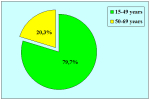
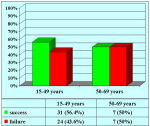
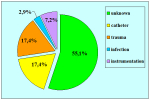
Summarizing table |
|||
Surgical Techniques: step by step
 Download PDF |